Cardiovascular disease is still a major cause of premature death in Australia. An important contributor to this burden is Sudden Cardiac death (SCD), which refers to a sudden lack of heart activity. Sudden cardiac death — also sudden cardiac arrest and unexplained cardiac death — is one of the biggest killers of Australians under 50 and is five times more likely to affect men. The primary cause of SCD in adults 35 and over is coronary heart disease. In younger people (under 35) it is congenital heart conditions and heart rhythm disorders.
It has been reported that in America researchers have found a genetic flaw that they believe is responsible for cases of sudden cardiac death (SDC), the biggest cause of death in the United States. It occurs when the heart simply stops beating or has no activity.
Although such stoppage can occur due to a heart attack, there is a type of SDC that occurs independent of heart disease. In such cases, the heart goes into an irregular heartbeat, or arrhythmia, causing it to flutter inefficiently and eventually stop.
There are a number of genes linked to arrhythmias, but it wasn’t previously known how these caused SDC. However, University of California Irvine researchers, using mice, discovered there is an impaired gene called KCNE2 that not only affects blood flow, but also activates chemical triggers that can cause SCD.
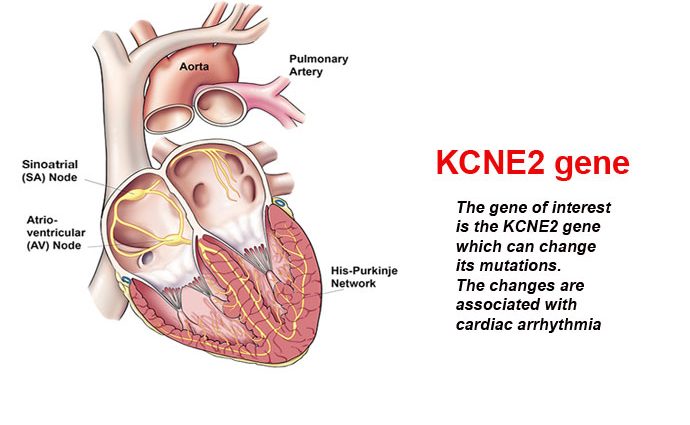
KCNE2 gene
potassium voltage-gated channel subfamily E regulatory subunit 2
Voltage-gated potassium (Kv) channels represent the most complex class of voltage-gated ion channels from both functional and structural standpoints. Their diverse functions include regulating neurotransmitter release, heart rate, insulin secretion, neuronal excitability, epithelial electrolyte transport, smooth muscle contraction, and cell volume. This gene encodes a member of the potassium channel, voltage-gated, isk-related subfamily. This member is a small integral membrane subunit that assembles with the KCNH2 gene product, a pore-forming protein, to alter its function. This gene is expressed in heart and muscle and the gene mutations are associated with cardiac arrhythmia.
University of California Irvine’s Geoffrey Abbott and his colleagues discovered that the functional impairment of a gene called KCNE2 underlies a multisystem syndrome that affects both heart rhythm and blood flow and can activate chemical triggers that can cause sudden cardiac death.
“With these findings, we can now explore improved early detection and prevention strategies for people who are at higher risk of sudden cardiac death, such as those with diabetes,” said Abbott, a professor of pharmacology and physiology & biophysics in the UC Irvine School of Medicine.
Study results appear in the February issue of Circulation: Cardiovascular Genetics, a publication of the American Heart Association.
Distinct from a heart attack, in which the heart continues to beat but blood flow is blocked, sudden cardiac death occurs when the heart ceases to beat because of the uncontrolled twitching of muscle fibers in its ventricles. Without defibrillation within minutes, this type of event is fatal.
In studies on a mouse model with the KCNE2 gene removed, Abbott and his colleagues had found catalysts for sudden cardiac death – including high blood cholesterol, anemia, high blood potassium, an age-related delay in the return to a resting position of the ventricle after contraction and, most surprisingly, diabetes.
The researchers are hoping their discovery will lead to a genetic test to discover those at risk of SDC and also pave the way for new treatments.